
by admin | Nov 14, 2017 | ACA, Group Benefit Plans, Human Resources, IRS
 October was a busy month in the employee benefits world. President Trump announced a new Acting Secretary for the U.S. Department of Health and Human Services (HHS). Eric Hargan fills the position vacated by Tom Price, who resigned in late September 2017. The U.S. Department of Labor (DOL) issued a proposed rule to delay a disability claims procedure regulation’s applicability date and HHS released its proposed rule on benefits and payment parameters for 2019. The U.S. Department of the Treasury (Treasury) issued its Priority Guidance Plan for projects it intends to complete during the first half of 2018.
October was a busy month in the employee benefits world. President Trump announced a new Acting Secretary for the U.S. Department of Health and Human Services (HHS). Eric Hargan fills the position vacated by Tom Price, who resigned in late September 2017. The U.S. Department of Labor (DOL) issued a proposed rule to delay a disability claims procedure regulation’s applicability date and HHS released its proposed rule on benefits and payment parameters for 2019. The U.S. Department of the Treasury (Treasury) issued its Priority Guidance Plan for projects it intends to complete during the first half of 2018.
DOL Proposes Delay to Final Disability Claims Procedures Regulations’ Applicability Date
The DOL issued a proposed rule to delay the applicability date of its final rule that amends the claims procedure requirements applicable to ERISA-covered employee benefit plans that provide disability benefits. The DOL’s Fact Sheet contains a summary of the final rule’s requirements.
The DOL is delaying the applicability date from January 1, 2018, to April 1, 2018, to consider whether to rescind, modify, or retain the regulations and to give the public an additional opportunity to submit comments and data concerning the final rule’s potential impact.
CMS Releases 2019 Benefits Payment and Parameters Proposed Rule
The Centers for Medicare & Medicaid Services (CMS) released a proposed rule and fact sheet for the 2019 Benefit Payment and Parameters. The proposed rule is intended to increase individual market flexibility, improve program integrity, and reduce regulatory burdens associated with the Patient Protection and Affordable Care Act (ACA) in many ways, including updates and annual provisions to:
- Essential health benefits
- Small Business Health Options Program (SHOP)
- Special enrollment periods (SEPs)
- Exemptions
- Termination effective dates
- Medical loss ratio (MLR)
CMS usually finalizes the Benefit Payment and Parameters rule in the first quarter of the year following the proposed rule’s release. November 27, 2017, is the due date for public comments on the proposed rule.
Almost all the topics addressed in the proposed rule would affect the individual market and the Exchanges, particularly the Small Business Health Options Program (SHOP) Exchanges.
Of interest to small group health plans, CMS proposes to change how states will select essential health benefits benchmark plans. If CMS keeps this change in its final rule, then it will affect non-grandfathered small group health plans for benefit years 2019 and beyond.
Treasury Issues its Priority Guidance Plan
The Treasury issued its 2017-2018 Priority Guidance Plan that lists projects that it intends to complete by June 30, 2018, including:
- Guidance on issues related to the employer shared responsibility provisions
- Regulations regarding the excise tax on high cost employer-provided coverage (“Cadillac tax”)
- Guidance on Qualified Small Employer Health Reimbursement Arrangements (QSE HRAs)
By Danielle Capilla
Originally Published By United Benefit Advisors

by admin | Nov 9, 2017 | ACA, Human Resources, IRS

Instructions for both the 1094-B and 1095-B and the 1094-C and 1095-C were released, as were the forms for 1094-B, 1095-B, 1094-C, and 1095-C.
Reporting will be due early in 2018, based on coverage in 2017. For calendar year 2017, Forms 1094-C, 1095-C, 1094-B, and 1095-B must be filed by February 28, 2018, or April 2, 2018, if filing electronically. Statements to employees must be furnished by January 31, 2018. In late 2016, a filing deadline was provided for forms due in early 2017, however it is unknown if that extension will be provided for forms due in early 2018. Until employers are told otherwise, they should plan on meeting the current deadlines.
All reporting will be for the 2017 calendar year, even for non-calendar year plans.
The reporting requirements are in Sections 6055 and 6056 of the ACA. The major reporting requirements are:
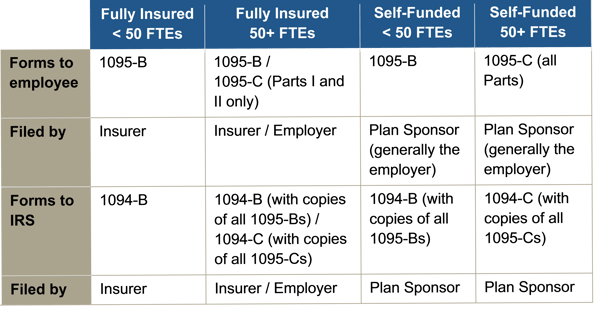

by admin | Nov 3, 2017 | Group Benefit Plans, HIPAA, Human Resources
 Employers who are designing a health and welfare benefit plan for their employees often wonder about the rules relating to setting premiums for employees. Employers generally have significant flexibility in this part of their plan’s design. Common structures contemplated by employers include, but are not limited to:
Employers who are designing a health and welfare benefit plan for their employees often wonder about the rules relating to setting premiums for employees. Employers generally have significant flexibility in this part of their plan’s design. Common structures contemplated by employers include, but are not limited to:
- Charging all employees a flat amount for their health plan
- Charging employees a percentage of the premium for the health plan, with the percentage changing as employees move between tiers (self, self plus one, self plus family)
- Giving employees a set dollar amount that they can use to offset the cost of whatever plan and plan tier they enroll in
Employers are also interested in setting different contribution structures for different groups of employees. Sometimes this is due to a geographic difference between employees, job types, staff versus management, and more. Employers may wish to give lower-paid employees more employer-provided money; sometimes employers wish to give managers or executive staff more employer-provided money.
Employers should be aware that there are different nondiscrimination requirements to consider.
Generally, under HIPAA non-discrimination rules, employers have discretion when structuring their benefits plans and may make distinctions among employee populations regarding access to and the level of benefits offered. Plans may differ among employees only on “bona fide employment-based classifications” consistent with the employer’s usual business practice. Examples that would satisfy this requirement include salaried, hourly, full-time, part-time, type of job, geographic location, date of hire, division, subsidiary, business unit, and profit center distinctions.
If an employer’s proposed structure meets these basic HIPAA requirements, then the employer needs to review the applicable nondiscrimination requirements under Internal Revenue Code Section 125 (for cafeteria plans) and Section 105(h) (for self-funded plans). If the employer’s plan is subject to these rules, at a most basic level, the plan cannot favor highly compensated individuals. Sometimes an innocent plan design can lead to an employer failing the nondiscrimination requirements under Section 125 or 105(h) without the employer intentionally favoring the highly compensated employees. Many employers also erroneously assume that none of their employees fall into the “highly compensated” category, so the rules do not apply to them. As a best practice, any time an employer has a plan design with different levels of employer contributions, the employer should run the applicable testing to ensure its plan is compliant.
Under Section 125, benefit plans cannot discriminate in favor of highly compensated individuals or key employees.
By Danielle Capilla
Originally Published By United Benefit Advisors

by admin | Oct 26, 2017 | Benefit Management, Benefit Plan Tips, Tricks and Traps, Human Resources

Fall. With it comes cooler temperatures’, falling leaves, warm seasonal scents like turkey and pumpkin pie, and Open Enrollment. It goes without saying; employees who understand the effectiveness of their benefits are much more pleased with those packages, happier with their employers, and more engaged in their work. So, as your company gears up for a new year of navigating Open Enrollment, here are a few points to keep in mind to make the process smoother for both employees and your benefits department. Bonus: it will lighten the load for both parties alike during an already stress-induced season.
Communicate Open Enrollment Using a Variety of Mediums
Advertise 2018 benefit changes to employees by using a variety of mediums. The more reminders and explanation of benefits staff members have using more than one mode of media, the more likely employees will go into Open Enrollment with more knowledge of your company’s benefit options and when they need to have these options completed for the new year.
- Consider explainer videos to simplify the amount of emails and paperwork individuals need to review come Open Enrollment time. These videos can increase the bottom line as well, eliminating the high cost of print material.
- Opt for placards placed throughout your high-traffic areas. Communicate benefit options and remind employees of Open Enrollment dates for the new year by posting in such areas as the lobby, break room and bathroom stalls.
- Choose SMS texting. Today, over 97% of individuals use text. Ninety-eight percent of those that use text open messages within the first three minutes of receiving them; 6-8 times higher than the engagement rate for email. Delivering a concise message to employees’ mobile devices creates more touch points along the Open Enrollment journey. The key, however, is making it quick so as to entice your employees to take action.
- Promote apps and in-app tools. Push notifications and apps like Remind 101 can help drive employee engagement during Open Enrollment season simply by providing short messages reminding them to enroll. Notifications like these can also be tailored to unique employee groups based on location, job level, eligibility status and more.
Utilize Mobile Apps and Web Portals for Open Enrollment
Now that your company has communication down pat for Open Enrollment, simplify the arduous task employees have of enrolling for the coming year by going paperless. Utilize web portals through benefit brokers and companies like ADP to eliminate the hassle of employees having to fill out paperwork both at renewal, and at the time of hire. With nearly three quarters of individuals in the United States checking their phone once an hour and 90% percent of this time is spent using one app or another as a main source of communication, mobile apps can make benefits engagement much easier due to the anywhere/anytime accessibility they offer.
The personal perks for employees are great too! Staff members with a major lifestyle event can make benefit adjustments quickly with the ease of mobile apps. Employees recognize this valuable and time-saving trend and enjoy having this information at their fingertips.
Open Enrollment season can be a stressful time but hopefully these tips will help for a smoother transition into the next year for your business. Simple things like using explainer videos, placing reminders in high traffic areas and utilizing mobile apps and text messaging can save time and stress in the long run for your employees and benefit department.

by admin | Oct 16, 2017 | Health & Wellness, Hot Topics, Human Resources
 There are places where you expect things to be noisy, such as a rock concert, and places where you expect it to be quiet, like an office. And while nobody likes being “shushed,” there are few things more annoying than trying to work when someone else is talking in the background.
There are places where you expect things to be noisy, such as a rock concert, and places where you expect it to be quiet, like an office. And while nobody likes being “shushed,” there are few things more annoying than trying to work when someone else is talking in the background.
The ‘80s music group ‘Til Tuesday said it best: “Hush hush, keep it down now, voices carry.” An article in Human Resource Executive Online titled, “A Not-So-Quiet Little Problem: Noise!,” points out the current problem of modern, open offices—NOISE. When offices had doors, or at least cubicles, along with sound-absorbing carpeting and ceiling tiles, background noise wasn’t such a problem. Now, however, offices are wide open with nothing to block sound waves. Combine that with hardwood, or concrete floors, lots of glass and tall, echoing ceilings, and you’ve got the perfect storm for noise pollution.
Forward-thinking, or technology companies especially like open offices, and you can imagine what it sounds like with people talking on the phone, banging away at their keyboards, and conversing with each other. According to the article, nobody considers the acoustics of a room. They look at how beautiful, modern, and spacious it is. Then, once the room is filled with busy employees, the shock of its lack of tranquility sets in.
Employees become distracted by the noise, which in turn leads to reduced productivity. You can tell a lot about the noise level of an office by how many employees are wearing headphones. For workers to feel “healthy” at work, noise is a major factor, along with air quality and temperature.
There are many ways to fix a noisy office if you follow the A, B, Cs—absorb, block, cover. Materials can be placed to absorb noise, walls or furniture can be positioned to block noise, and there are electronic devices that use counter-measures to cover noise. The industry, office layout, and other factors will influence the choice of the best solution to mitigate noise. One thing is certain: when choosing a new office, or remodeling an existing one, it’s best to factor in a room’s acoustics along with its aesthetics.
By Geoff Mukhtar
Originally posted by www.UBABenefits.com

by admin | Sep 27, 2017 | Benefit Plan Tips, Tricks and Traps, Employee Benefits, Human Resources
 We’ve all been there – once or twice (or more)—when a child, spouse or family member has had to gain access to healthcare quickly. Whether a fall that requires stitches; a sprained or broken bone; or something more serious, it can be difficult to identify which avenue to take when it comes to walk-in care. With the recent boom in stand-alone ERs (Emergency Care Clinics or ECCs), as well as, Urgent Care Clinics (UCCs) it’s easy to see why almost 50% of diagnoses could have been treated for less money and time with the latter.
We’ve all been there – once or twice (or more)—when a child, spouse or family member has had to gain access to healthcare quickly. Whether a fall that requires stitches; a sprained or broken bone; or something more serious, it can be difficult to identify which avenue to take when it comes to walk-in care. With the recent boom in stand-alone ERs (Emergency Care Clinics or ECCs), as well as, Urgent Care Clinics (UCCs) it’s easy to see why almost 50% of diagnoses could have been treated for less money and time with the latter.
It’s key to educate yourself and your employees on the difference between the two so as not to get pummeled by high medical costs.
- Most Emergency Care facilities are open 24 hours a day; whereas Urgent Care may be open a maximum of 12 hours, extending into late evening. Both are staffed with a physician, nurse practitioners, and physician assistants, however, stand alone ECCs specialize in life-threatening conditions and injuries that require more advanced technology and highly trained medical personnel to diagnose and treat than a traditional Urgent Care clinic.
- Most individual ERs charge a higher price for the visit – generally 3-5 times higher than a normal Urgent Care visit would cost. The American Board of Emergency Medicine (ABEM) physicians’ bill at a higher rate than typical Family-Medicine trained Urgent Care physicians do (American Board of Family Medicine (ABFM). These bill rates are based on insurance CPT codes. For example, a trip to the neighborhood ER for strep throat may cost you more than a visit to a UC facility. Your co-insurance fee for a sprain or strain at the same location may cost you $150 in lieu of $40 at a traditional Urgent Care facility.
- Stand alone ER facilities may often be covered under your plan, but some of the “ancillary” services (just like visit rates) may be billed higher than Urgent Care facilities. At times, this has caused many “financial sticker shock” when they first see those medical bills. The New England Journal of Medicine indicates 1 of every 5 patients experience this sticker shock. In fact, 22% of the patients who went to an ECC covered by their insurance plan later found certain ancillary services were not covered, or covered for less. These services were out-of-network, therefore charged a higher fee for the same services offered in both facilities.
So, what can you and your employees do to make sure you don’t get duped into additional costs?
- Identify the difference between when you need urgent or emergency care.
- Know your insurance policy. Review the definition of terms and what portion your policy covers with regard to deductibles and co-pays for each of these facilities.
- Pay attention to detail. Understand key terms that define the difference between these two walk-in clinics. Most Emergency Care facilities operate as stand-alone ERs, which can further confuse patients when they need immediate care. If these centers, or their paperwork, has the word “emergency”, “emergency” or anything related to it, they’ll operate and bill like an ER with their services. Watch for clinics that offer both services in one place. Often, it’s very easy to disguise their practices as an Urgent Care facility, but again due to CPT codes and the medical boards they have the right to charge more. Read the fine print.
It’s beneficial as an employer to educate your employees on this difference, as the more they know – the lower the cost will be for the employer and employee come renewal time.

 October was a busy month in the employee benefits world. President Trump announced a new Acting Secretary for the U.S. Department of Health and Human Services (HHS). Eric Hargan fills the position vacated by Tom Price, who resigned in late September 2017. The U.S. Department of Labor (DOL) issued a proposed rule to delay a disability claims procedure regulation’s applicability date and HHS released its proposed rule on benefits and payment parameters for 2019. The U.S. Department of the Treasury (Treasury) issued its Priority Guidance Plan for projects it intends to complete during the first half of 2018.
October was a busy month in the employee benefits world. President Trump announced a new Acting Secretary for the U.S. Department of Health and Human Services (HHS). Eric Hargan fills the position vacated by Tom Price, who resigned in late September 2017. The U.S. Department of Labor (DOL) issued a proposed rule to delay a disability claims procedure regulation’s applicability date and HHS released its proposed rule on benefits and payment parameters for 2019. The U.S. Department of the Treasury (Treasury) issued its Priority Guidance Plan for projects it intends to complete during the first half of 2018.





